If patients are undergoing long-term IV therapy, regular assessment must be done to monitor any possible complications.
Intravenous fluid regulation, otherwise known as IV therapy, is a medical technique for administering fluids, nutrition, or medications into a patient’s bloodstream. This practice has been around in healthcare centers and hospitals for decades as a means to provide a quick and smooth infusion of medicinal fluids to patients.
There are several reasons IV therapy is performed. In fact, around 80% of patients in all hospitals are bound to receive IV therapy as part of their treatment plans.
Some of the common reasons IV therapy is performed on patients may include:
- To provide medications for infections and other diseases
- To treat dehydration by replacing fluids and maintaining the body’s electrolyte balance
- To donate or administer blood which is required, especially during major surgeries
- To provide additional nutrients to the body through fluid nutritional supplements
- To treat cancer by administering chemotherapy drugs
Intravenous therapy may also be administered to patients who cannot take their medications orally due to emergency situations.
IV Therapy Regulations Established In The United States
The fluid used for each treatment consists of medication, electrolytes, and glucose, wherein the amount of concentration depends on the patient’s specific needs. The amount and quantity of IV fluid given to the patient will also depend on their age, body size, and medical condition. Administering the correct amount of fluid in the patient’s bloodstream is extremely important to avoid complications from receiving excessive or inadequate amounts.
Furthermore, over the years, more businesses and aesthetic facilities have been attempting to provide quick and easy IV therapy to their clients via IV Bars, allowing them easy access to IV treatments and infusions of vitamins. Unfortunately, many of these business owners fail to realize the risk and dangers of errors associated with IV infusions and therapies.
Thus, certain regulations and general guidelines were developed in the United States to ensure medical practitioners and healthcare professionals know what to do when performing IV therapy. Remember, IV therapy is an invasive medical procedure which means the risk of complications is very high when incorrect medication or the wrong amount of fluid is given to the patient.
This article will present the following IV therapy regulations established in the U.S.
- Intravenous therapy should only be ordered by a licensed physician or nurse
The Corporate Practice of Medicine (CPOM) generally prohibits businesses and non-physicians from administering IV therapy. After a patient undergoes a proper diagnosis in a hospital or healthcare center, only a licensed doctor may prescribe IV therapy.
The doctor will determine the type of fluid required for the patient’s treatment and particular condition. Along with that, the prescription must also include the duration of the therapy, the rate of infusion, and the date and time it shall start. An assigned professional nurse shall then be the one to disinfect the patient’s skin.
It’s also imperative that nurses and licensed doctors must have the proper apparatus for administering IV therapy. Different IV administration sets may be required, depending on the patient’s needs and medical situation. The IV device set may include the catheter (needle), a flow regulator, an infusion line filter, tubing, connectors, a hollow spike, an IV set stopcock, and an infusion fluid container.
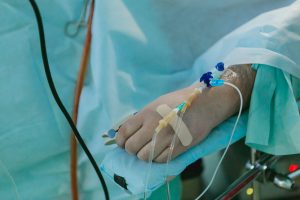
Using the wrong device during the injection process may cause infiltration, in which the fluid or medication injected leaks outside the bloodstream, causing tissue damage. Furthermore, according to research, another side effect of the wrong usage of IV devices is phlebitis, or inflammation of the veins. Around 31% of hospital patients have experienced phlebitis, so inform your doctor right away if you encounter symptoms like pain, swelling, and irritation on the injection site.
- Aseptic technique must be observed throughout all IV therapy procedures
With IV therapy being an invasive medical procedure, the risk of infection and contamination is also very high. Thus, healthcare professionals must observe the aseptic technique throughout the whole IV therapy procedure.
To do this, physicians or nurse practitioners must first prepare, disinfect, and sterilize all the IV administration sets. They’ll need to check all the apparatus for any sign of damage, expiration, or moisture penetration. IV therapy devices must be appropriately stored away from areas with a high risk of contamination. It’s also essential to avoid reusing single-use items and dispose of them properly right after use.
The healthcare staff and practitioners following the aseptic technique must have proof that they’re free from any illnesses or infections (e.g., cough, sore throat, fever). They must also wear proper clothing with a disposable apron, perform proper hand hygiene and wear sterile gloves prior to handling any IV equipment. Overall, observing the aseptic technique will reduce the risk of bacteria contaminating the IV equipment and possibly infecting the patients.
- Understand the indications of IV therapy complications.
A few complications and minor risks will likely happen to some patients during IV therapy. Some minor complications may include:
- Swelling or irritation on the injection site
- Collapsed vein
- Dislodged IV catheter
- Fluid overload
- Complications related to the quantity or type of medication given
Thankfully, these risks can be treated and prevented as long as practitioners understand the signs and indications of IV therapy complications. Thus, healthcare practitioners must be aware of the special needs of their patients undergoing IV therapy.
If patients are undergoing long-term IV therapy, regular assessment must be done to monitor any possible complications. When fluid overload occurs, the patient may show symptoms such as anxiety, trouble breathing, and headache. Patients must immediately alert their doctor or nurse to check their flow rate if they’re experiencing any of these symptoms during IV therapy.
The Bottom Line
Overall, intravenous therapy is common and generally safe. The regulations and guidelines of IV therapy in the U.S. are purposely established to ensure all licensed and qualified healthcare practitioners continue to provide high-quality care and IV treatment to their patients. Most importantly, knowing the fact that healthcare professionals are following these regulations will give patients the utmost confidence in receiving IV therapy.


Join the conversation!