The medical community is experimenting with different treatment methods to combat addiction crisis.
In an effort to combat opioid addiction, medical professionals once followed standardized protocols for administering buprenorphine, a leading opioid treatment drug, to patients hooked on heroin. However, the rise of fentanyl, a potent opioid that has flooded the market in recent years, has presented a new set of challenges. Unlike heroin, fentanyl is up to 50 times more powerful and requires a more delicate approach when initiating buprenorphine treatment. As doctors in Washington State grapple with this issue, they find themselves in uncharted territory, experimenting with various methods to find the best solutions for their patients.
Dr. Nate Kittle, an addiction care overseer at HealthPoint, a nonprofit organization operating clinics throughout King County, highlights the lack of universally accepted treatment protocols for fentanyl addiction. He acknowledged that practitioners often rely on word-of-mouth and local practices, given the absence of established guidelines. Dr. Kittle states, “We’re still learning the best ways to do this.”
One approach to combat addiction, known as microdosing, involves slowly increasing the amount of buprenorphine a patient receives to avoid intense withdrawal symptoms. However, Dr. Kittle points out that this method is complicated and has a relatively low success rate. Patients often fear taking larger doses of buprenorphine due to potential withdrawal, leading them to remain trapped in their addiction.
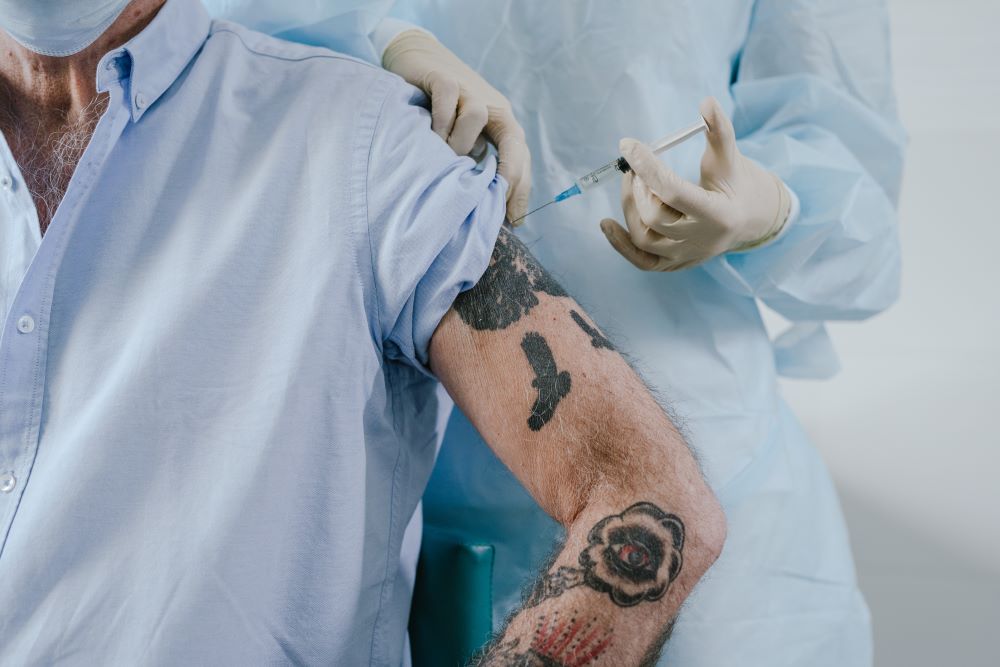
On the other hand, some emergency room doctors are advocating for macrodosing, which entails providing large doses of buprenorphine to patients on the first day of treatment.
Surprisingly, many patients do not experience precipitated withdrawal, contrary to what was previously assumed. Dr. Mark Duncan, a UW Medicine psychiatrist involved in addiction treatment, noted that many assumptions about treatment effectiveness have been challenged through these real-world experiences.
Yet another approach to combat addiction gaining traction is the use of long-acting medications like Sublocade. This injection slowly releases buprenorphine over a month, eliminating the need for daily doses and the constant reminder of addiction inevitably present with more frequent treatments. Dr. Duncan has observed remarkable success with Sublocade, especially for individuals struggling with fentanyl addiction.
Despite these promising treatments, the medical community is cautious about implementing them. Dr. Lily Lo from a Centralia drug treatment clinic explained, “We don’t want to make somebody sick. Our first role is to do no harm.” Balancing the benefits with potential risks is a critical consideration in this ever-evolving field.
Furthermore, some physicians are exploring unconventional methods to ease the transition to buprenorphine. Dr. Lucinda Grande has been experimenting with using small doses of ketamine, an anesthetic with hallucinogenic effects, to alleviate withdrawal symptoms. While this method shows promise, its widespread utility remains uncertain, primarily due to challenges in accessing and using ketamine.
Amidst the ongoing search for effective fentanyl addiction treatments, the medical community remains committed to finding safe and compassionate approaches. As Dr. Duncan tracks patient experiences and shares insights with his peers, the hope is that a collective effort will lead to improved protocols and better outcomes for those struggling with fentanyl addiction.
As renowned addiction specialist Dr. Michael Levy once said, “Addressing addiction is not just about finding the right medication or therapy; it’s about understanding the individual’s unique struggles and tailoring the treatment accordingly.”
Sources:
WA doctors detail pros, cons of fentanyl addiction treatment methods
Microdosing: A Guide to Using Buprenorphine During the Illicit Fentanyl Pandemic
Method for Successfully Inducting Individuals Who Use Illicit Fentanyl Onto Buprenorphine/Naloxone

Join the conversation!