MMS reaches a $18M settlement with the Department of Justice in whistleblower case.
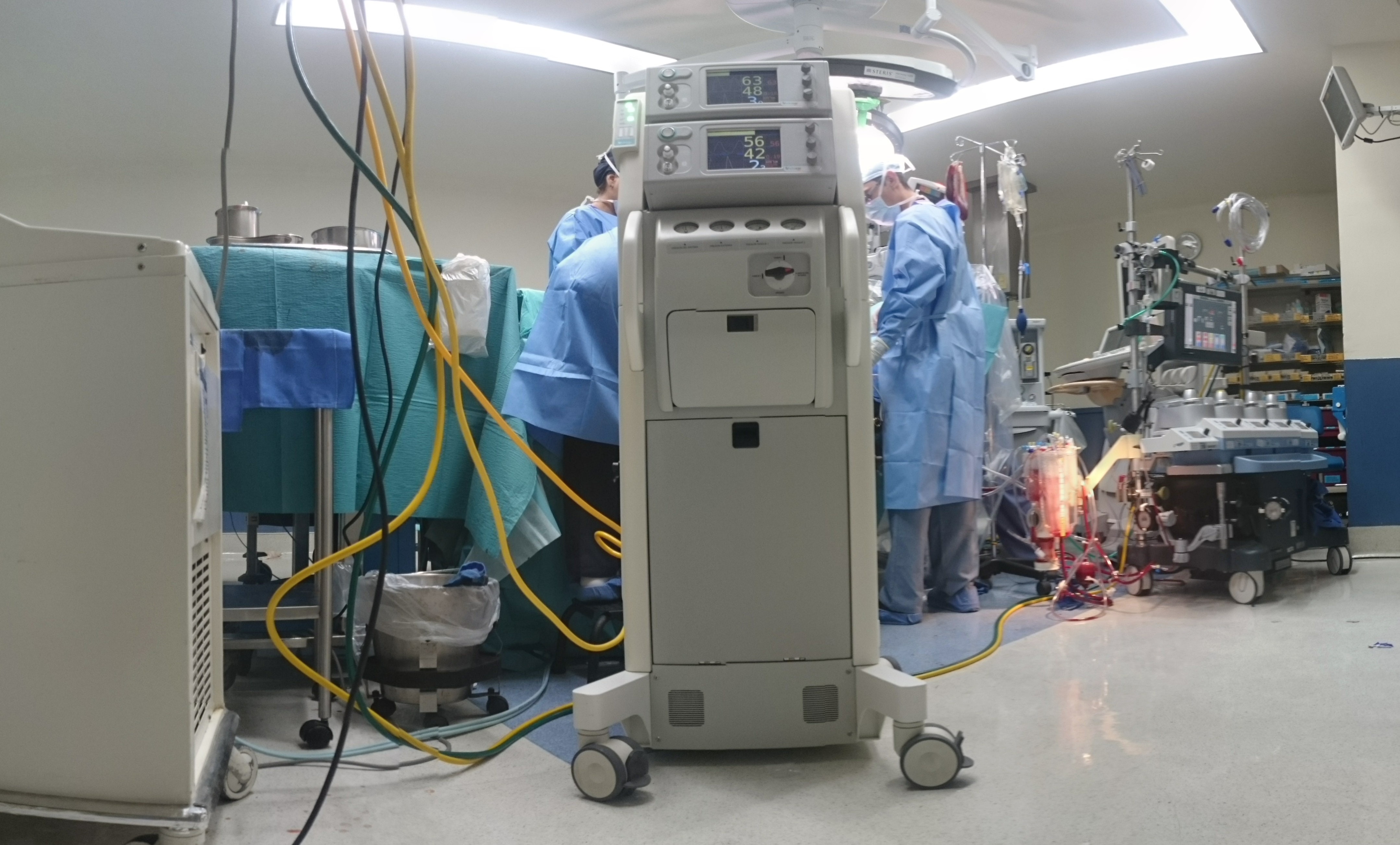
Merit Medical Systems (MMS) has agreed to pay $18 million to resolve allegations that it submitted false claims to Medicare, Medicaid, and TRICARE by paying kickbacks to physicians and hospitals to use its products. MMS makes disposable medical devices used in a variety of medical procedures. Its devices have been used in cardiology, radiology, oncology, critical care and endoscopy.
The anti-kickback statute prohibits companies from offering to pay to induce the referral of items covered by Medicare, Medicaid and TRICARE. The AKS statute is designed to ensure medical providers use devices in their practices based on objective decision-making without receiving financial incentives.
A whistleblower lawsuit was filed in 2016 exposing the kickback scheme involving paying physicians and facilities to use MMS’ product line. Former chief compliance officer, Dr. Charles J. Wolf, was the whistleblower whose suit claimed the company was in violation of the False Claims Act. He filed after submitting his resignation that April and received $2.65 million of the federal share of the settlement. Wolf argued he made “repeated efforts to address violations that he said were deeply ingrained in Merit’s culture.” Documents contend, “Despite these clear and persistent warnings, MMS ignored these concerns and continued with the illegal payment system.”
Merit Medical officials, Wolf claimed, “also wined and dined doctors, sent them on trips to extravagant locations, and paid them exorbitant consulting fees for little or no work” in order to “gain market share at inflated prices” and to get them to buy more Merit products. The lawsuit further stated MMS used “fraudulent advertising disguised as educational grants as well as inflated writing and speaking fees and other cash as inducements to physicians and hospitals to use several of its specialty medical devices.”
Court records show MMS rolled out an internal program, Local Advertising Program, “which provided health care providers millions of dollars in free advertising, practice development, practice support and unrestricted ‘educational” grants,” the lawsuit contends, and states further, “MMS selected health care providers for these payments based on prior sales.”
“Federal and state law prohibit payments to physicians intended to influence their choice of medical devices,” said Veronica Nannis, an attorney with the law firm Joseph Greenwald & Laake, which represented Wolf. “When medical device companies pay something of value to induce physicians to use their devices to the exclusion of others, that can effect independent medical judgment and patient care.”
Along with the False Claims Act settlement, MMS agreed to a five-year Corporate Integrity Agreement with the Department of Health and Human Services’ Office of Inspector General (HHS-OIG), in which it must hire a compliance expert and an independent review organization to keep an eye on its operations.
Merit founder, chairman and CEO Fred Lampropoulos confirmed a settlement with the Department of Justice (DOJ) had been reached. “Given the mounting costs and time demands associated with the investigation, we believe this resolution is in the best interest of the business,” Lampropoulos said. “Merit will continue to focus on our core mission: To be the most customer-friendly company in health care.”
Sources:
Merit Medical Systems Settles False Claims Act Case for $18 Million
Utah-based Merit Medical to pay $18 million settlement in lawsuit claiming doctor kickbacks

Join the conversation!